
Research into full mouth reconstruction in Orlando often begins with visible concerns such as worn teeth, repeated fractures, difficulty chewing, or restorations that no longer feel stable. What is less obvious is how dentists determine whether comprehensive treatment is necessary. Full mouth reconstruction is not recommended based on appearance alone, nor is it suggested for isolated problems that can be addressed conservatively.
Instead, the decision is grounded in structural patterns, bite function, and long-term stability. Dentists evaluate how teeth interact, whether forces are distributed evenly, and whether cumulative damage suggests a broader imbalance within the mouth. When multiple factors point toward instability rather than a single repairable issue, a comprehensive approach may be considered. Understanding how this evaluation works helps explain why a full mouth reconstruction is sometimes recommended and why, in other cases, a more conservative path is appropriate.

Full mouth reconstruction refers to rebuilding or restoring most or all teeth in both the upper and lower arches when widespread damage affects function and stability. Treatment plans often combine restorative procedures, such as crowns, bridges, dental implants, periodontal therapy, and occlusal adjustments, to strengthen compromised teeth and reestablish balanced contact between the arches.
This approach is recommended when structural breakdown, missing teeth, or bite collapse interfere with comfort and daily function. The goal is to create a stable foundation that supports efficient chewing, protects remaining tooth structure, and distributes forces evenly across the bite.
While aesthetic improvements often result from alignment and proportion corrections, the primary focus remains on restoring mechanical balance and long-term durability rather than cosmetic enhancement alone.
Before discussing treatment options, dentists conduct a detailed clinical assessment. This process identifies patterns that may not be immediately visible.
Previous restorations, repeated fractures, and patterns of wear offer important clues. A history of crowns that repeatedly fail or fillings that crack under pressure may indicate an imbalance in bite forces. Reviewing past treatment helps determine whether prior care addressed underlying mechanics or simply managed symptoms.
Jaw fatigue, tension headaches, uneven tooth wear, or difficulty chewing may signal broader structural stress. These concerns guide further diagnostic steps and help clarify whether isolated repairs will provide long-term stability.
Structural assessment focuses on the condition of existing teeth.
Dentists look for:
When deterioration affects multiple teeth rather than a single isolated area, repairing each tooth individually may not address the root cause. Reconstruction can provide a coordinated strategy that restores harmony across the entire arch.
Bite alignment — known as occlusion — plays a central role in determining candidacy.
Even small discrepancies in how teeth meet can create uneven force distribution. Over time, this imbalance may lead to fractures, sensitivity, or muscle strain. Dentists evaluate how the upper and lower arches interact during speaking, chewing, and resting positions.
Signs of bite imbalance may include:
When bite instability affects multiple teeth, comprehensive correction may provide greater predictability than repeated localized repairs.
Visual examination alone cannot reveal every structural concern. Advanced imaging provides essential information.
Digital radiographs and three-dimensional scans allow dentists to evaluate:
Imaging ensures that recommendations are based on structural reality rather than surface appearance.
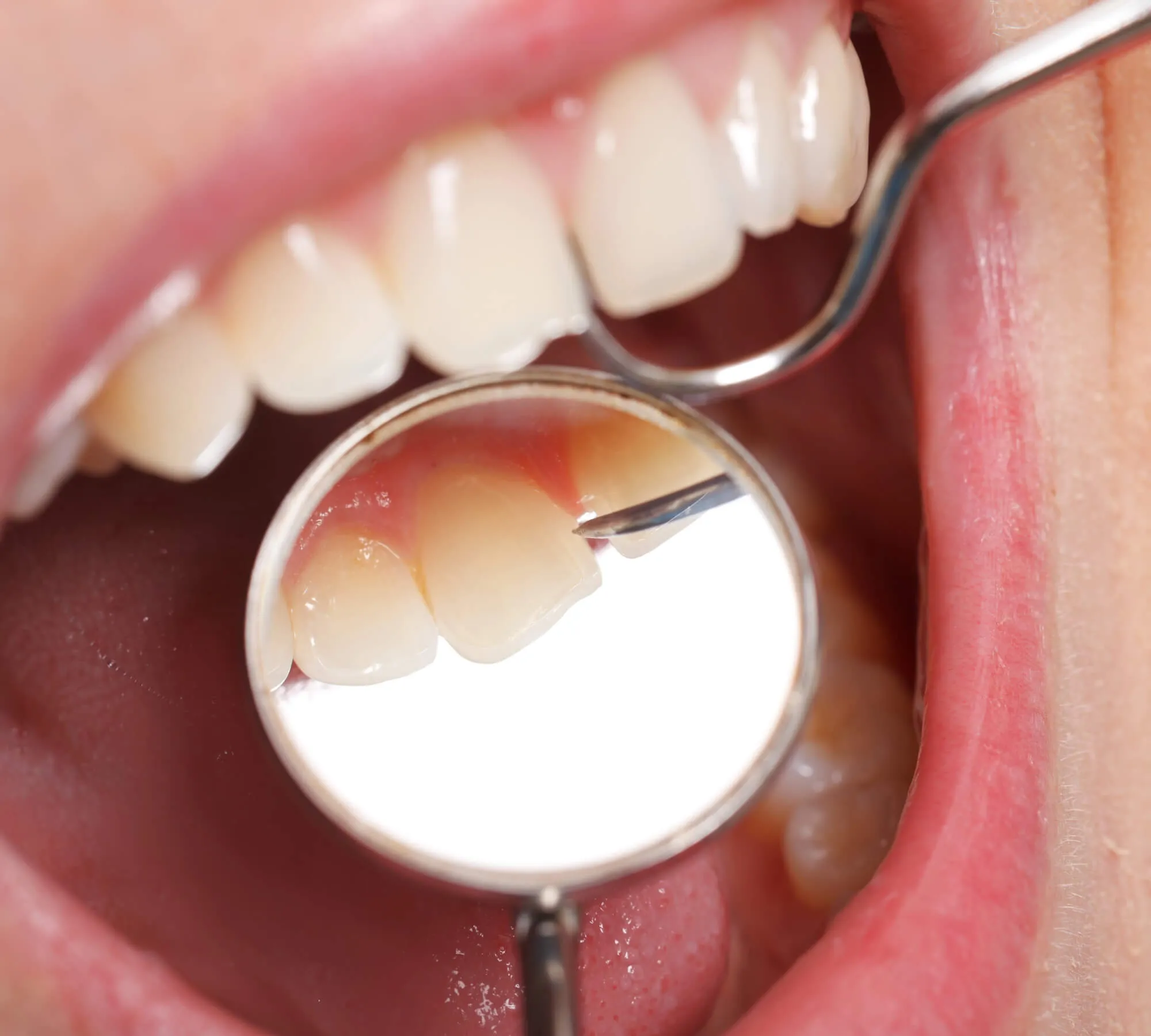
In some situations, individual restorations can improve comfort temporarily but do not resolve the underlying imbalance affecting the entire bite. For example:
When structural stress continues across multiple areas, isolated repairs often become cyclical rather than corrective. Replacing one restoration at a time may manage symptoms but fail to stabilize the overall system. In these cases, dentists evaluate whether ongoing patchwork treatment will provide predictable long-term support or whether a coordinated reconstruction plan would better protect the remaining teeth and reestablish functional balance across the arches.
Full mouth reconstruction is typically recommended when function is compromised. Indicators may include:
Addressing these concerns often requires recalibrating the bite rather than treating individual teeth in isolation.
Gum health and bone support are foundational. Active periodontal disease must be stabilized before restorative treatment begins. Bone levels are assessed to determine whether teeth can be preserved or require replacement. Healthy supporting structures improve predictability and longevity.
Full mouth reconstruction is a structured, methodically process that is typically completed in carefully planned stages to support accuracy and stability.
This initial stage focuses on creating a healthy foundation. It may involve treating active infection, managing gum inflammation, addressing periodontal concerns, or removing teeth that cannot be preserved. The goal is to eliminate factors that could interfere with long-term success.
During this phase, teeth are rebuilt or replaced with restorations such as crowns, bridges, or implants. Bite height and alignment may be adjusted to distribute forces more evenly and restore functional balance.
Permanent restorations are placed once healing, stability, and alignment are confirmed.
Phased planning allows time for healing, careful monitoring, and necessary refinements throughout treatment.
Comprehensive treatment is not always necessary. When damage is limited to one or two teeth and bite alignment remains stable, conservative care may be sufficient.
Responsible planning includes recognizing when a localized solution is appropriate.
Every case is unique. Tooth anatomy, facial structure, jaw position, and muscle activity influence planning decisions.
Dentists consider:
Reconstruction is customized rather than standardized. Careful evaluation prevents overtreatment while supporting structural stability.
Durability after full mouth reconstruction depends on consistent care and ongoing evaluation. Protective appliances, such as night guards, may be recommended for patients who grind or clench to reduce excessive force on restorations. Maintaining balanced bite forces helps protect both natural teeth and newly placed restorations.
Routine dental visits play an important role in monitoring stability. During these appointments, dentists assess bite alignment, evaluate the integrity of crowns or implants, and check gum health. Early identification of minor changes allows for timely adjustments before complications develop. While reconstruction establishes a stable foundation, regular maintenance helps preserve function, comfort, and structural balance over time.
Full mouth reconstruction is a structured response to cumulative structural imbalance. It is not recommended solely based on cosmetic preference or isolated discomfort.
Dentists assess biomechanics, structural integrity, and long-term stability before recommending comprehensive care. This careful analysis reduces uncertainty and improves predictability.
When supported by clinical findings, reconstruction can restore function, evenly distribute forces, and protect remaining tooth structure.
If you are considering full mouth reconstruction, a consultation provides clarity about whether this approach aligns with your oral health needs. A comprehensive evaluation allows time to assess structural damage, bite alignment, bone support, and overall stability before determining the most appropriate plan.
At Altamonte Implant & Cosmetic Dentistry, treatment planning focuses on detailed analysis, phased care, and long-term function. Scheduling a consultation offers the opportunity to review findings, discuss options, and understand whether comprehensive reconstruction or a more conservative approach best supports your goals.