When patients begin researching affordable dental implants in Orlando, they often focus on appearance, cost, or treatment timelines. While those factors matter, one of the most important parts of implant success happens beneath the surface. Understanding the biological process that allows implants to function like natural teeth can help patients make informed decisions.
At the center of implant stability is a process called osseointegration. Though the term may sound technical, the concept is straightforward. Osseointegration refers to the process by which the jawbone gradually bonds to the surface of a dental implant after it is placed. This biological connection is what allows implants to remain stable and support everyday functions like chewing and speaking.

Osseointegration is the process by which living bone forms a direct structural connection with the surface of a titanium implant. The term combines “os,” the Latin word for bone, with “integration,” meaning to make whole or unite.
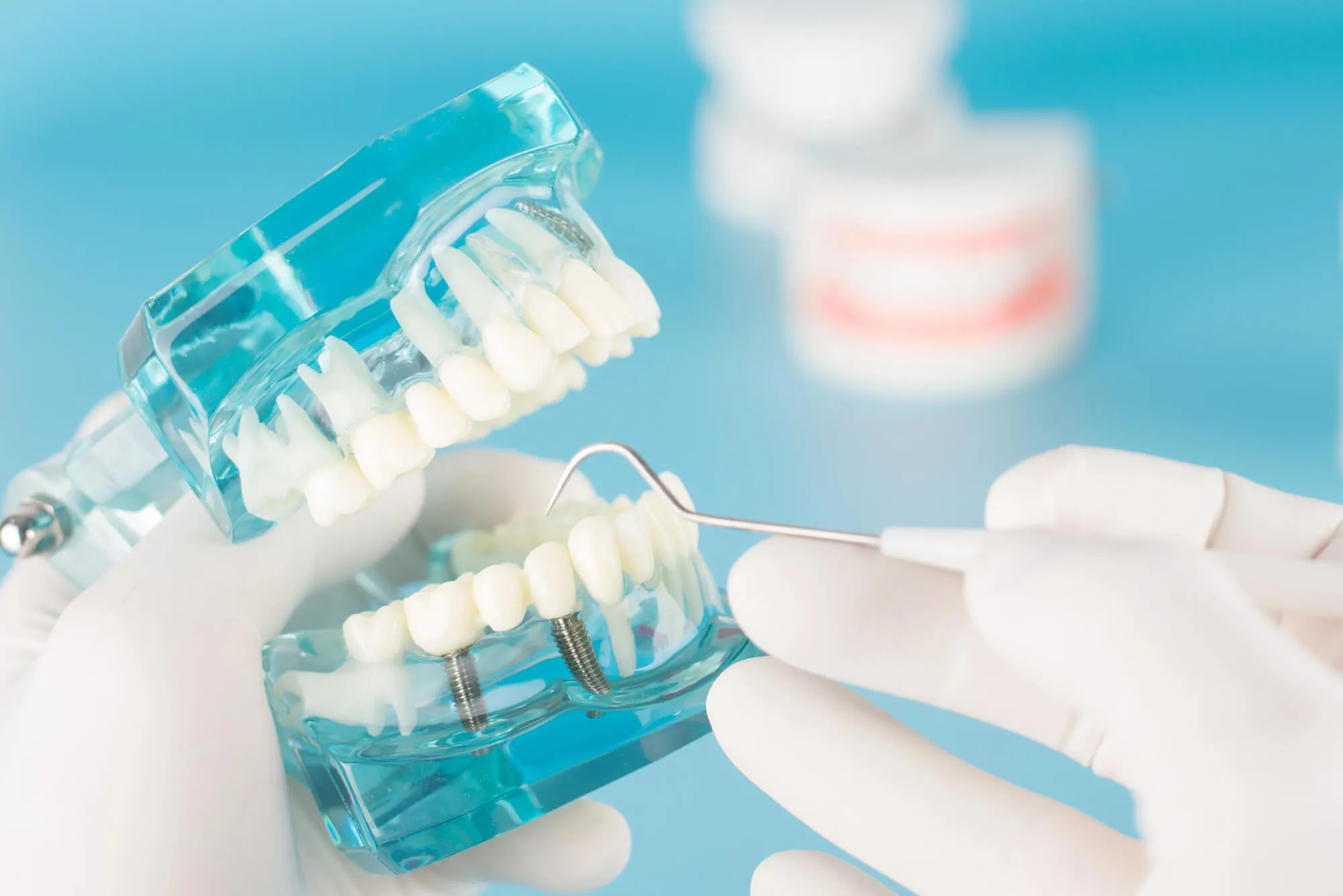
Dental implants are usually made of biocompatible titanium or titanium alloys. These materials are chosen because they are well tolerated by the body and form a stable bond with bone tissue. Unlike removable options that rest on the gums, implants are anchored in the jawbone.
This bond is not created through glue or cement. Instead, it is a natural biological response.
Once the implant is placed, the surrounding bone begins to remodel and adapt around its surface. Over time, this creates a stable foundation that can support a crown, bridge, or full-arch restoration.
Titanium has been used in medical applications for decades because of its compatibility with human bone. When titanium is placed in bone, it forms a thin oxide layer on its surface. This layer helps bone cells attach and grow.
Modern implants are designed with textured or treated surfaces that increase the surface area available for bone contact. This design encourages stronger attachment during the healing process. The surface does not fuse in a way that changes the metal itself; instead, bone cells grow into microscopic irregularities, creating mechanical stability.
This interaction between bone and titanium is what makes dental implants different from other tooth replacement options.
Osseointegration does not occur immediately after implant placement. Instead, it develops gradually through a series of biological stages that allow the jawbone to adapt to the implant surface.
After placement, the body responds with a normal inflammatory process. Blood cells, proteins, and growth factors move to the surgical site to begin tissue repair. During this phase, a blood clot forms around the implant, serving as the foundation for new bone development. Early stability at this stage depends largely on how precisely and securely the implant was positioned within the existing bone.
As healing progresses, specialized bone-forming cells called osteoblasts begin producing new bone along the implant surface. At the same time, osteoclasts reshape and remove older bone tissue. This coordinated remodeling allows the jaw to adapt structurally to the implant.
Over the following months, the bone-implant interface strengthens. As mineralization continues, stability increases. Once sufficient integration is confirmed, a final restoration may be placed.
Although patients may feel comfortable within weeks, biological integration continues quietly beneath the surface for several months.
Osseointegration is predictable in most healthy individuals, but several factors can influence its efficiency and reliability. Understanding these variables helps explain why treatment planning and follow-up care are tailored to each patient.
Bone density plays a significant role in initial implant stability. Denser bone often provides stronger mechanical support at the time of placement, which can support early healing. Softer or thinner bone may still allow successful integration but may require additional planning, modified techniques, or a longer healing period.
Healthy gum tissue helps create a protective barrier around the implant. Active periodontal disease or untreated inflammation may increase bacterial presence near the implant site, which can interfere with early healing and long-term stability.
Certain systemic health conditions, including uncontrolled diabetes or disorders affecting bone metabolism, may influence how the body forms new bone. Some medications that alter bone turnover may also impact healing.
Smoking has been associated with delayed healing and a higher risk of implant complications. While it does not automatically prevent placement, it often requires closer monitoring.
Excessive biting pressure, clenching, or grinding during early healing can affect stability. Dentists evaluate and adjust bite alignment to reduce unnecessary stress.
Once integrated, the implant becomes a stable part of the jaw structure. This stability allows implants to:
Unlike removable appliances, implants help stimulate the jawbone through regular function. When teeth are missing, the jawbone may gradually lose density due to a lack of stimulation. Implants help reduce that risk by transferring chewing forces into the bone.
Patients sometimes assume that once an implant feels comfortable, healing is complete. In reality, biological integration continues beyond what can be felt.
Placing a final restoration too soon may subject the implant to stress before bone adaptation is sufficient. That is why dentists use imaging, stability testing, and clinical evaluation before progressing to the next phase of treatment.
Even when discussing dental implants, the biological process remains the same. Cost considerations do not change the need for proper healing and evaluation.
While implant success rates are high in healthy patients, osseointegration is not automatic. Failure to integrate can occur if the implant does not achieve sufficient stability or if infection interferes with healing.
Common causes of early implant complications may include:
If integration does not occur as expected, the implant may need to be removed and replaced after healing. Careful planning and follow-up help reduce these risks.
Monitoring involves:
These evaluations allow dentists to determine when the implant is ready to support long-term restoration.
Patients who understand osseointegration often approach implant treatment with more realistic expectations. Healing is not about speed alone. It is about creating a stable biological foundation that can last for many years.
When researching dental implants, it is helpful to remember that successful outcomes depend on careful planning, proper healing time, and professional monitoring. The science behind integration does not change based on pricing models—it relies on biology and precision.
When integration is successful, implants can:
With appropriate care and regular dental visits, implants can remain stable for many years.
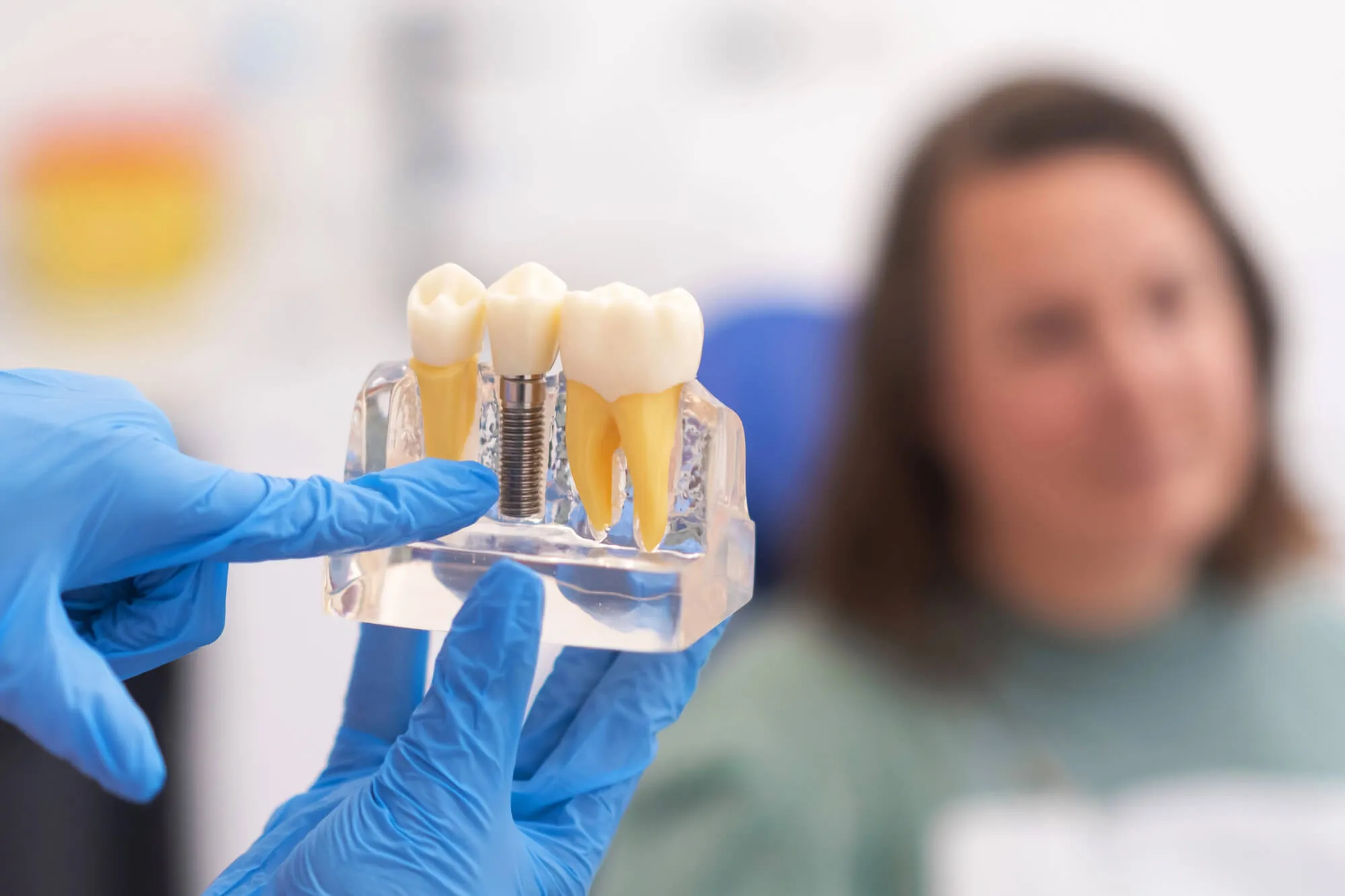
Osseointegration is the foundation that allows dental implants to remain stable and function predictably over time. While the process happens beneath the surface, its success depends on careful placement, healthy bone, and guided healing. Understanding how bone adapts to an implant helps explain why planning, monitoring, and follow-up care are essential parts of treatment—not just the procedure itself.
If you are exploring affordable dental implants in Orlando, a consultation provides the opportunity to evaluate bone health, discuss healing timelines, and understand how implant stability is assessed throughout each phase of care.
At Altamonte Implant & Cosmetic Dentistry, treatment planning focuses on precision, communication, and long-term stability. Scheduling a consultation allows you to review your options and determine the most appropriate path forward for your needs.